Benefits of Dental Implants
For those who are missing teeth, it is important to get the issue taken care of as soon as possible. There are a number of disadvantages to missing teeth including trouble speaking, trouble eating properly, an increased risk for gum disease and, of course, feeling self-conscious. When individuals decide it is time to take care of their missing teeth, it is important to work with a qualified dental care professional.
What Are My Treatment Options?
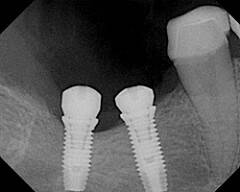
There are three common treatments that are used by dental professionals to correct an issue with missing teeth – implants, dentures, and bridges. Dental implants are placed into the bone socket of the tooth that is missing and over a period of time the jawbone will grow around the implant. Dentures can be done either as a partial or full denture, which is attached to a plastic base and are removable. Finally, bridges are an artificial tooth that is positioned between two crowns.
What Are the Advantages of Using Dental Implants?
While all three of the above mentioned treatments are common, dental implants have a number of advantages dentures and bridges cannot offer. First, dental implants provide individuals with more natural function – after the implant bonds with the jaw bone, they fake tooth feels no different than the individual’s natural teeth. Additionally, dental implants require little to no maintenance, which means the individual will spend less time worry about their implant and less time in the dentist’s chair.
Some other benefits offered by dental implants include stability and longevity of the tooth as well as helping to keep the other teeth in place. Those individuals who opt for a dental implant often find that the implant helps to support and protect the surrounding teeth and also keeps the other teeth from sifting. Bridges, for example, although supported by the natural teeth on either side, often require the individual to have the teeth on the sides of the bridge filed down in order to fit correctly.
Missing teeth is a serious dental health issue that should not be ignored or taken lightly. If you experience tooth loss, it is important to visit a dental care professional as soon as possible to discuss possible treatment options and which treatment is right for the patient and their lifestyle. Dental implants are often the right choice, given the stability, longevity, and low maintenance of the implant.
If you are avoiding a needed procedure because of cost, you need to consider the Wellness Dental Plan. Our plan is a New Hampshire discount dental plan offering as much as 20 percent off all emergency and routine dental care. For more information, please click here.
*Photo Courtesy of Mike Stanley via Creative Commons License